Types of Integrative Medicine

Jump ahead to these answers:
- What Is Ayurveda or Ayurvedic Medicine?
- What Is Placebo Therapy?
- What Is Traditional Chinese Medicine?
- What Is Virtual Reality Therapy?
- What Is Psychedelic-Assisted Therapy?
- What Is Art Therapy?
- What Are Biofield Therapies?
- What Is Music Therapy?
- What Is Aromatherapy?
- What Are Tai Chi and Qigong?
- What Is Mindfulness-Based Stress Reduction?
- What Is Meditation?
- What Is Yoga?
- What Is Spinal Manipulation?
- What Is Acupuncture?
What Is Ayurveda or Ayurvedic Medicine?
July 8th, 2025Ayurveda, or Ayurvedic medicine, is a traditional and holistic medical system that originated in India over 5,000 years ago. It is one of the oldest medical systems in the world and continues to be a traditional healthcare system in modern India. The term Ayurveda is derived from Sanskrit and means science of life. Ayurveda focuses on the prevention and treatment of illness through balancing the mind, body, and consciousness with an appropriate diet, lifestyle, and the use of herbs.
Ayurvedic beliefs indicate that every individual has three energy types (doshas) which are known as vata, pitta, and kapha. Each energy controls a specific function in the body. Vata dosha controls functions associated with motion; pitta dosha controls the metabolic systems, and kapha dosha controls growth. When these energies are unbalanced, they can cause illness or negative emotional responses. Unbalanced vata results in anxiety and fear; unbalanced pitta results in anger and ulcers; and unbalanced kapha results in envy and insecurity. Energy balance can be negatively affected by factors such as unhealthy eating habits, stress, poor family relationships, or the weather. Ayurvedic treatments address these imbalances to help restore health and well-being.
There have been a few clinical trials and studies with findings that have suggested Ayurvedic treatments are effective for concerns such as knee pain, arthritis symptoms, type 2 diabetes, and some aspects of ulcerative colitis and cancer. However, some findings have also shown that the safety of Ayurvedic products can be questionable since some may include high levels of lead, heavy metals, mercury, and arsenic. It should be noted that around 20% of Ayurvedic medicines are classified as Rasashastra, which combines gems, metals, and minerals as the ingredients. Among these Ayurvedic medicines, some purposely contain lead or mercury as part of the treatment. Being mindful of this, individuals interested in Ayurvedic medicine are encouraged to consult with their physician to examine the benefits and risks associated with its use.
Sources
“Ayurveda”. Mount Sinai. https://www.mountsinai.org/health-library/treatment/ayurveda
“Ayurvedic Medicine: In Depth”. National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/ayurvedic-medicine-in-depth
“What is Ayurveda and Does It Work?”. Cleveland Clinic. https://health.clevelandclinic.org/what-is-ayurveda
What Is Placebo Therapy?
July 8th, 2025A placebo is any treatment with no therapeutic value or active properties. Placebo therapy can include tablets known as sugar pills, injections that only contain saline solution, or even sham surgeries that omit a therapeutically necessary step in the process. When patients experience a change or improvement after being given a placebo, this is known as a placebo effect. In clinical trials for pharmaceuticals, researchers use placebos to determine and evaluate the efficacy of new medications.
While placebos don’t have any actual substances or properties to them, they still have the potential to improve symptoms, often due to the patient’s belief that they are receiving effective treatment for their condition. Since they lack therapeutic value, they aren’t able to cure medical conditions. Still, they can be helpful in the management of the symptoms associated with those conditions. For example, a placebo cannot cure cancer. But it can help relieve the symptoms of nausea and fatigue. Placebos may also be helpful in pain management and relieving the symptoms of stress-induced insomnia.
Although there is a stigma surrounding the use of placebos in healthcare, the positive outcomes associated with the placebo effect may still provide comfort and symptom relief to individuals who might otherwise fail to experience improvement with traditional forms of medicine. Some of these positive outcomes may be associated with the hopeful expectations of the patients and the fact that they are receiving medical care, which may convince the brain that the treatment is real and effective. In any case, it’s important to consider the placebo’s ability to produce the desired outcome and relief, especially if it reduces distress among patients with end-stage disease. Eventually, scientists may harness the effects of placebos to herald a new type of care that relies less on pharmacological interventions while emphasizing psychosocial interactions and the power of the mind.
Sources
“The Power of the Placebo Effect”. Harvard Health. https://www.health.harvard.edu/mental-health/the-power-of-the-placebo-effect
““Consensus on Placebo and Nocebo Effects Connects Science with Practice:” Reply to “Questioning the Consensus on Placebo and Nocebo Effects” Karger. https://karger.com/pps/article/90/3/213/294358/Consensus-on-Placebo-and-Nocebo-Effects-Connects
“The neuroscience of placebo effects: connecting context, learning and health”. Nature Reviews Neuroscience. https://www.nature.com/articles/nrn3976
What Is Traditional Chinese Medicine?
July 8th, 2025Traditional Chinese Medicine (TCM) is a holistic medical system practiced for thousands of years throughout China and other parts of East Asia. It is based on the belief that the body’s vital energy, called “Qi,” flows through channels in the body to keep an individual’s emotional, mental, spiritual, and physical health in constant balance. The use of TCM aims to balance the body between two forces, yin and yang. Yin is characterized by negative and cold energy, whereas yang is characterized by positive and warm energy. Although both forces exist opposite of each other, they are interconnected and complementary to Qi. If there is a disruption or imbalance in the flow of Qi, the individual will experience illness or chronic disease.
Since traditional Chinese medicine is a medical system, it consists of various therapeutic practices. These practices include but are not limited to Chinese herbal medicine, acupuncture, cupping, qigong, and tai chi. Each of these practices aims to restore the balance of Qi in the body to promote health and well-being.
Acupuncture involves inserting thin needles in any of the over 2,000 identified points in the body to improve the flow of Qi, which should relieve discomfort. Practices such as qigong and tai chi focus on poses, breathing patterns, and movement to reduce the amount of qi stuck or stagnant in the body’s channels. Another method of removing stagnated qi is cupping, which uses small cups to achieve a suction effect on the skin, resulting in the breaking of blood vessels to stimulate healing.
Chinese herbal medicine uses specific herbs in the form of capsules, granules, tea, powder, liquid extracts, or combined into a formula. Some formulas are traditional and have been used for thousands of years. In contrast, others are customized based on the individual’s unique needs. The focus of using Chinese herbal medicine is not to treat disease but to address individual signs and symptoms of the imbalance in the body to optimize health and well-being. Individuals interested in being treated with Chinese herbal medicine are encouraged to talk with their physician first and, if approved, have a formal consultation with a licensed herbalist who is board-certified in traditional Chinese herbal medicine.
Sources
“Complementary and Alternative Medicine”. National Cancer Institute. https://www.cancer.gov/about-cancer/treatment/cam
“What Is Traditional Chinese Medicine?” Cleveland Clinic. https://health.clevelandclinic.org/chinese-medicine
“Acupuncture”. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/wellness-and-prevention/acupuncture
“An Introduction to Qigong”. Cleveland Clinic. https://health.clevelandclinic.org/what-are-the-health-benefits-of-qigong
“Slow and Steady: The Health Benefits of Tai Chi”. Cleveland Clinic. https://health.clevelandclinic.org/the-health-benefits-of-tai-chi
“Cupping Therapy”. Cleveland Clinic. https://my.clevelandclinic.org/health/treatments/16554-cupping
“What You Should Know About Chinese Herbs”. Cleveland Clinic. https://health.clevelandclinic.org/what-you-should-know-about-chinese-herbs
What Is Virtual Reality Therapy?
July 8th, 2025Virtual reality therapy is an innovative therapeutic intervention that uses technology to create immersive simulated environments, ultimately enabling patients to participate in settings and activities that they might otherwise not be able to experience due to physical limitations. Although virtual reality therapy continues to be a focus of research in a variety of contexts, it has been shown to have promising implications for use among patients at the end of life since it provides a unique source of distraction and relief from anxiety and distress. Studies have also found that VRT may reduce pain and improve the quality of life for terminally ill patients.
VR therapy is a powerful intervention since it can engage patients through multiple senses to provide a truly immersive experience. The use of equipment such as headsets in combination with 360° panoramic videos and open worlds can introduce patients to settings and environments that are vividly realistic. It may be used in conjunction with relaxation or mindfulness techniques for additional benefit, although some use cases focus more directly on the experience of these visually immersive settings to promote positive emotions, develop a sense of comfort or confidence, or even fulfill final wishes.
Common use cases for VRT have included overcoming phobias, easing chronic pain, and navigating psychiatric disorders such as depression, anxiety, and PTSD. A limited number of providers are trained in using VRT since it is a fairly new form of therapy, but this is likely to change as the technology continues to improve and become more accessible. VRT costs tend to vary based on insurance coverage, the provider, and whether patients are expected to purchase headsets or other equipment. Some healthcare facilities maintain multiple headsets and other equipment to ensure that they are accessible for patients determined to be a good fit for this level of intervention.
It is important to understand that the field of VR therapy is actively evolving and will require additional research to fully understand the potential long-term implications and applications in different settings. Integrating VR experiences specifically tailored to patient needs and preferences may further enhance its therapeutic benefits. It would also significantly expand the possibilities for patients to experience different aspects of their bucket lists. Ultimately, VRT may be a valuable therapeutic tool and source of final cherished memories with loved ones at the end of life.
Sources
“The use of virtual reality technology in the treatment of anxiety and other psychiatric disorders.” National Library of Medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5421394/
“Virtual reality therapy: Everything you need to know.” Forbes Health. https://www.forbes.com/health/mind/virtual-reality-therapy/
“Virtual reality reduces pain in palliative care–A feasibility trial.” BMC Palliative Care. https://bmcpalliatcare.biomedcentral.com/articles/10.1186/s12904-022-01058-4
What Is Psychedelic-Assisted Therapy?
July 8th, 2025Psychedelic-assisted therapy is the newly rediscovered technique of using psychedelic substances such as psilocybin and LSD to help patients achieve mental health goals. Patients are given low to moderate doses of a psychedelic substance in a controlled setting under the supervision of a medical or mental health professional and then observed as the experience unfolds. Later, the patient and therapist meet to discuss the experience in a process called “integration,” during which they talk about what the experience was like and what it meant. A second session following the same protocol is usually scheduled within one to two weeks.
Although deceptively simple in design, psychedelic therapy has proven to have remarkable benefits for a wide array of mental health conditions. Below is a short summary of just a few recent studies and their results:
Post-traumatic stress disorder
A recent Phase 3 clinical trial conducted by the Multidisciplinary Association of Psychedelic Studies, or MAPS, treated 90 patients with severe, chronic PTSD with MDMA (ecstasy). After three sessions, 67% of patients no longer met the criteria for PTSD, and 88% had achieved significant reduction of PTSD symptoms. This held true even for those subjects who had comorbidities such as depression and substance abuse.
Distress associated with terminal illness
Multiple studies have demonstrated a significant reduction in symptoms of depression and anxiety in terminally ill patients treated with psilocybin. Patients in these studies have also reported improvements in quality of life, optimism, death acceptance and spiritual connection following the treatment experience. Additionally, a recent study at Johns Hopkins University School of Medicine using a single dose of high-dose psilocybin in patients with terminal cancer showed significant reductions in depression and anxiety in approximately 80% of subjects both immediately after the experience and at a six-month follow-up.
Depression
A small phase 2 clinical trial conducted in London and reported in the New England Journal of Medicine compared the efficacy of two doses of psilocybin to daily dosing of the antidepressant escitalopram (Lexapro) for the treatment of long-standing major depressive disorder. Of the 59 patients in the study, those who received psilocybin had at least as great or a greater decrease in self-reported depressive symptoms than those in the antidepressant group. This study builds on prior research that has shown psilocybin therapy to nearly eliminate depressive symptoms in a majority of patients with chronic major depressive disorder.
The results of these and other studies are so promising that the Food and Drug Administration recently designated psilocybin as a breakthrough therapy and approved a large-scale clinical trial for its use in major depression. MAPS has also requested breakthrough status for MDMA in the treatment of PTSD.
Sources
“LSD”. Drugs.com. https://www.drugs.com/illicit/lsd.html
“What Is Psychedelic Therapy?” VeryWell Mind. https://www.verywellmind.com/psychedelic-therapy-how-does-it-work-5079161
“Treating PTSD with MDMA Assisted Therapy”. Multidisciplinary Association for Psychedelic Studies. https://maps.org/2021/05/03/maps-phase-3-trial-of-mdma-assisted-therapy-for-ptsd-achieves-successful-results-for-patients-with-severe-chronic-ptsd/
“Policy Statement and Review: Psilocybin Therapy for Emotional Suffering Caused by Terminal Illness”. End of Life Washington. https://endoflifewa.org/news/policy-statement-and-review-psilocybin-therapy-for-emotional-suffering-caused-by-terminal-illness/
“Psilocybin produces substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer: A randomized double-blind trial”. Journal of Psychopharmacology. https://pmc.ncbi.nlm.nih.gov/articles/PMC5367557/
“Trial of Psilocybin versus Escitalopram for Depression”. The New England Journal of Medicine. https://www.nejm.org/doi/full/10.1056/NEJMoa2032994
“Psychedelic Treatment with Psilocybin Relieves Major Depression, Study Shows”. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/news/newsroom/news-releases/2020/11/psychedelic-treatment-with-psilocybin-relieves-major-depression-study-shows
“Breakthrough Therapy”. U.S. Food and Drug Administration. https://www.fda.gov/patients/fast-track-breakthrough-therapy-accelerated-approval-priority-review/breakthrough-therapy
What Is Art Therapy?
July 8th, 2025Art therapy is the practice of making art under the guidance of a trained professional who has completed a master’s degree and received special training in both the creative process and psychology. Art therapists work in conjunction with mental health providers, doctors, nurses and other clinicians in various settings to help clients meet a variety of therapeutic goals. These include but aren’t limited to the following:
- Exploring their feelings
- Developing self-awareness
- Managing undesirable behaviors such as addictions
- Developing social skills
- Reducing anxiety
- Reconciling emotional conflicts
- Coping with trauma, including grief and loss
- Managing stress and distress
The field of art therapy was first introduced in the U.S. in the 1940s, when Margaret Naumburg, a psychologist with an interest in art, and Edith Kramer, an artist who had a deep regard for Freud’s psychoanalytic theory, joined forces. Together, they developed a process that used art-making as a way to help clients express their thoughts and feelings through creative expression. Since that time, the practice has gained popularity, both with mental health professionals and medical providers. The techniques used can be applied in a variety of situations, including the following:
- Children who have suffered trauma or abuse
- Children who are having behavioral problems at home or at school
- Adults who have experienced a trauma or traumatic loss
- Adults or children living with a serious illness
- Older adults who are struggling with loneliness, infirmity, and physical challenges associated with advancing age
Art therapy has also been used — typically in conjunction with other Integrative techniques such as music therapy and meditation — in hospice and palliative care. Various studies involving people with cancer have shown that engaging with art in a variety of ways helps patients focus more on positive life experiences, maintain an identity apart from their diagnosis and develop emotional resilience. Art therapy has also been shown to help dying patients with meaning-making and to provide an outlet for feelings of anxiety and existential dread. Patients with dementia have also shown improvements in mental acuity, social interaction and levels of depression when they engaged in art therapy consistently over time.
Sources
“The Connection Between Art, Healing, and Public Health: A Review of Current Literature”. American Journal of Public Health. https://ajph.aphapublications.org/doi/10.2105/AJPH.2008.156497
“Art Therapy and Creative Coping Techniques for Older Adults”. https://books.google.com/books?id=OJLy_3RRqE4C&pg=PA251&dq=art+help+clients+communicate,+overcome+stress,+and+explore+different+aspects+of+their+own+personalities.&hl=en&sa=X&ved=2ahUKEwiM8feMkajkAhVEuVkKHWPBA48Q6AEwAnoECAIQAg#v=onepage&q=art%20&f=false
What Are Biofield Therapies?
July 8th, 2025Biofield therapies are noninvasive techniques in which a practitioner interacts with another’s biofield (also called an energy field or aura) with the goal of rebalancing vital energy to facilitate healing, improve well-being and address specific health concerns. Also referred to as “energy healing,” biofield therapies have been practiced across the globe for thousands of years, but only in the past few decades have they become accepted in the Western world. Although many variations on the techniques exist, those most commonly practiced in the U.S. are Reiki, Therapeutic Touch, and Healing Touch. Below we give a brief overview of each one.
Reiki
The term “Reiki” is derived from two Japanese words: “rei,” which means universal, and “ki,” which means energy (also referred to as “qi”) and translates roughly to “mysterious energy” in English. The practice began in Japan thousands of years ago, but the form of Reiki used most often today was introduced by Usui Sensei in 1922. The practice came to the U.S. in the 1940s and Europe in the 1980s. According to a 2014 report from the Washington Post, the technique is offered in at least 60 hospitals in the U.S., and demand among patients is growing every year.
In a typical Reiki session, a practitioner, known as a Reiki master, uses their hands to interact with the client’s energy field. During some Reiki sessions, the practitioner will touch the client, while in others they just hold their hands a few inches above the client’s body. The hands are held in position until they feel warm to the touch, indicating that movement of “stuck” energy has occurred. Some Reiki sessions are done from a distance of many miles away.
The benefits of Reiki, like all biofield therapies, have not been established scientifically. But patients and practitioners say it works. The main benefit, they claim, is a profound sense of relaxation and greater well-being. Reiki has not been shown to have an effect on any disease processes, although some anecdotal reports say it helps alleviate pain.
Therapeutic Touch
Developed in the 1970s by Dolores Krieger, Ph.D, R.N, of New York University, and Dora Kunz, a natural healer, Therapeutic Touch is very similar to Reiki in that it involves the balancing of a client’s energy field using the hands. Therapeutic touch practitioners place their hands a few inches above the client’s body and move them from head to toe, sensing where energy is stuck or blocked. Once they have made this assessment, they use a practice called “clearing” or “unruffling,” in which they move their hands up, down and across the client’s body in a rhythmic way to balance the energy field.
There have been numerous studies conducted on the benefits of Therapeutic Touch, either alone or in combination with other Integrative therapies. Most of these have shown that Therapeutic Touch promotes deep relaxation, decreases anxiety and helps to relieve physical pain in postoperative patients and people with osteoarthritis or burns. It has also been shown to stimulate cell growth, which may aid in wound healing and improve function in patients with connective tissue disorders such as arthritis. The deep relaxation achieved by people who receive therapeutic touch has also been shown to improve sleep quality and overall well-being in elderly patients receiving palliative care.
Healing Touch
Very similar in most aspects to both Reiki and Therapeutic Touch, Healing Touch is a technique in which a practitioner uses their hands to sense energy imbalances in a person’s body and moves them in specific ways to re-establish energy flow so that the client can heal. Research has shown that the practice can achieve the following:
- Reduce anxiety
- Alleviate stress
- Reduce symptoms of depression, particularly in patients with cancer
- Reduce the perception of physical pain
- Enhance feelings of hope and well-being
Originally taught as a continuing education course for nurses and massage therapists, Healing Touch is now part of the curriculum at many universities, nursing schools and medical schools.
Sources
“What is the History of Reiki?”. The International Center for Reiki Training. https://www.reiki.org/faqs/what-history-reiki
“Research – Creating and supporting the development and evolution of Therapeutic Touch”. Therapeutic Touch International Association. https://therapeutictouch.org/about-us/research/
“Therapeutic Touch(®) in a geriatric Palliative Care Unit – A retrospective review”. Complementary Therapies in Clinical Practice. https://pubmed.ncbi.nlm.nih.gov/27502814/
“What is Healing Touch?” Healing Beyond Borders. https://www.healingbeyondborders.org/index.php/what-is-healing-touch
What Is Music Therapy?
July 8th, 2025Music therapy is a therapeutic tool in which a specially trained music therapist develops individualized interventions to meet specific patient goals. Music therapists complete a college degree in music therapy and an internship, after which they are eligible to sit for a certification exam offered by the Certification Board for Music Therapists. Those who pass the exam are then board-certified music therapists and may work in a variety of settings, including hospitals, nursing homes, mental health facilities, prisons and schools.
Music therapy as a discipline includes a wide array of interventions and techniques, including the following:
- Music improvisation
- Receptive music listening
- Songwriting
- Singing
- Music-assisted relaxation
- Music and guided imagery
- Movement to music
- Music and massage
It has many applications in clinical practice, including symptom management for people living with chronic illnesses such as cancer, heart disease and HIV; elderly persons with dementia or Alzheimer’s disease; and those living with mental illness such as depression, anxiety or schizophrenia. It has also proven useful in palliative care and hospice. According to a literature review published in the journal Evidence-Based Complementary and Alternative Medicine in 2005, music therapy may help patients at the end of life manage symptoms such as pain, fatigue and anxiety, and improve their mood and overall quality of life.
Music at the bedside of the dying
With that being said, music can be therapeutic even when it is not part of a formal intervention by a board-certified music therapist. Many hospitals, hospices and outpatient settings offer live music performed by paid musicians or volunteers as a means of creating a more healing environment for patients, visitors and staff. Bedside Harp, for example, partners with several hospitals on the East Coast to offer harp music at the bedside of terminally ill and dying patients and also trains staff and interested volunteers in the art of playing the bedside harp. And Threshold Choir, a 501(c)3 nonprofit with over 200 chapters across the U.S., has offered sung music at the bedside of those hovering between life and death since 2001. Members visit the dying in groups of two to four, performing soft, soothing harmonies that comfort both the dying person and their grieving loved ones.
Sources
“Music Therapy in Hospice and Palliative Care: A Review of the Empirical Data”. Evidence-Based Complementary and Alternative Medicine. https://onlinelibrary.wiley.com/doi/10.1093/ecam/neh076
“Our Founding Story”. Bedside Harp. https://www.bedsideharp.com/about/
Threshold Choir. https://thresholdchoir.org/
What Is Aromatherapy?
July 8th, 2025Aromatherapy is the therapeutic use of essential oils extracted from plants. Each essential oil has a different chemical makeup that affects how it smells, how it is absorbed and how it is used by the body.
Some of the oils most commonly used in aromatherapy include:
- Roman chamomile
- Geranium
- Lavender
- Tea tree
- Lemon
- Ginger
- Cedarwood
- Bergamot
Aromatherapy may be employed in several different ways. According to the National Cancer Institute, these include the following:
- Indirect inhalation, in which the oil is placed in a diffuser and dispersed throughout the patient’s room. The oils may also be placed on a tissue or cotton ball and placed next to the patient’s bed or chair.
- Direct inhalation, in which a patient uses an inhaler that uses a few drops of essential oil set atop hot water.
- Massage, in which one or more essential oils is added to a carrier oil and massaged into the skin.
One of the most common uses of aromatherapy is to relieve stress and anxiety. According to Hopkins Medicine, the scent of inhaled oils travels through the olfactory nerves directly to an area of the brain known as the amygdala, which processes fear-inducing stimuli. This action may be responsible for its calming effect. However, this premise hasn’t been proven scientifically. Moreover, a study conducted by the National Center for Complementary and Integrative Health found no change in biochemical markers, immune function or other stress indicators in individuals who received aromatherapy while under stress.
Essential oils have also been shown to have antidepressant qualities, particularly in people with cancer. And according to Dr. Brent A. Bauer, director of the Department of Internal Medicine’s Complementary and Integrative Medicine Program at Mayo Clinic in Rochester, Minnesota, the use of lavender oil specifically may help to reduce pain due to osteoarthritis of the knee, improve sleep quality in people with dementia and help alleviate pain from kidney stones.
Aromatherapy is also used in combination with other Integrative health approaches to improve the quality of life for people with cancer. According to the National Cancer Institute, many cancer patients find that aromatherapy helps to relieve stress and anxiety and reduce chemotherapy-related nausea and vomiting. Aromatherapy is also widely employed in hospice and palliative care.
Sources
“Aromatherapy With Essential Oils (PDQ®)–Patient Version”. National Cancer Institute. https://www.cancer.gov/about-cancer/treatment/cam/patient/aromatherapy-pdq#link/_45
“A Review on the Effects of Aromatherapy for Patients with Depressive Symptoms”. The Journal of Alternative and Complementary Medicine. https://www.liebertpub.com/doi/abs/10.1089/acm.2008.0333?2=
“Home Remedies: What are the benefits of aromatherapy?”. Mayo Clinic. https://newsnetwork.mayoclinic.org/discussion/home-remedies-what-are-the-benefits-of-aromatherapy/
“Aromatherapy”. National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/aromatherapy
“Aromatherapy: Do Essential Oils Really Work?” Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/wellness-and-prevention/aromatherapy-do-essential-oils-really-work
What Are Tai Chi and Qigong?
July 8th, 2025According to WebMD, tai chi and qigong are closely related, centuries-old practices that combine slow, coordinated movements with meditation and breathing techniques. Tai chi was initially developed as a martial art similar to judo and karate, but has evolved into a slower practice that is used to improve physical and emotional health. The focus is on moving the entire body in a prescribed fashion in patterns similar to those seen in nature.
Qigong, on the other hand, is a more contemplative practice — some refer to it as the “internal process” of tai chi. Literally translated as “energy work” or energy cultivation, the aim of qigong is to move energy through the body in a specific way with a specific goal. Thus, the movements are more static and are performed repeatedly in sequence, usually three, six or nine times.
Cate Morrill, a tai chi and qigong instructor at Piedmont Healthcare Cancer Wellness, explains the difference between the two this way: “Think of a weightlifter who focuses on building his or her biceps with biceps curls. The weightlifter repeats those curls to build the muscle, focusing on that muscle only. In the same way, qi gong focuses on a particular issue in the mind, body or spirit,” she says. “Tai chi, on the other hand, has more similarities to a full-body weightlifting routine.”
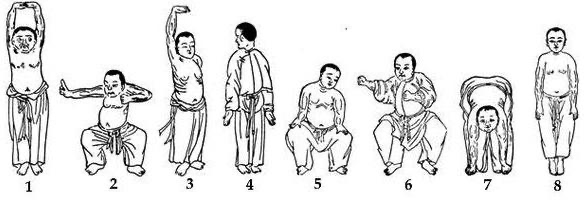
One of the simplest forms of qigong, Baduanjin qigong, incorporates only eight movements, sometimes called the Eight Pieces of Brocade. Photo-Public Domain
With that being said, in actual practice, qigong and tai chi are remarkably similar, at least as they are performed in the Western world. And they have similar health benefits, according to the National Center for Complementary and Integrative Health. For example, both practices achieve the following:
- Improve balance and stability in the elderly and people with Parkinson’s disease
- Improve flexibility
- Reduce back pain
- Reduce pain associated with osteoarthritis of the knee
- Improve quality of life for people with cancer, heart disease and other serious illnesses
- Improve thinking, problem solving, reasoning and memory in seniors who showed no evidence of cognitive decline and those with mild cognitive impairment (tai chi only).
What’s more, both forms of exercise are low-impact and easy on the joints, so they are well-suited to people who are elderly or living with chronic conditions such as osteoarthritis.
Sources
“Tai Chi and Qi Gong”. WebMD. https://www.webmd.com/fitness-exercise/tai-chi-and-chi-gong
“The difference between tai chi and qi gong”. Piedmont. https://www.piedmont.org/living-real-change/the-difference-between-tai-chi-and-qi-gong
“Tai Chi: What You Need To Know”. National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/tai-chi-what-you-need-to-know
What Is Mindfulness-Based Stress Reduction?
July 8th, 2025In Western culture, one of the most popular and most studied forms of meditation is mindfulness-based stress reduction, a technique started in 1979 by Jon Kabat Zinn, Ph.D., professor of medicine emeritus at the University of Massachusetts Medical School. The deceptively simple practice includes two main components: attention to breath and the body scan (sequentially bringing attention to different parts of the body). Originally developed as an eight-week in-person course taught at the Center for Mindfulness at UMass Memorial Medical Center, the practice is based on a series of techniques, including a sitting meditation, a walking meditation, yoga and a 45-minute body scan. Since its inception, MBSR has been adopted by health care providers across the world as a means of helping people living with various forms of chronic illness manage stress and distress in their everyday lives. The Center for Mindfulness also currently offers online access to bi-weekly mediation sessions on its website, which are free to attend.
Since Kabat-Zinn introduced the idea of using mindfulness as an adjunct to conventional medical treatment, three decades of research have substantiated its beneficial effects. Some of the most notable of these include the following:
- A 41% reduction in mortality after two years in patients who added MSBR to a standard cardiac rehabilitation regimen for the treatment of coronary artery disease. Cardiac rehab patients in the MBSR program also experienced less psychological distress and better overall health, as indicated by greater weight loss, improved lipid profiles and lower blood pressure, than those treated with standard care alone.
- Reduced blood pressure in people with hypertension. These reductions were comparable to those achieved with medication and lifestyle changes such as weight loss, salt restriction and increased exercise.
- A substantial reduction (65%) in symptoms of anxiety, depression, anger and confusion in cancer patients along with a 30% decrease in physical symptoms associated with stress. In one study, survival rates of patients with melanoma and metastatic breast cancer also improved with the introduction of MBSR.
- Significant improvement in both the experience of pain and the overall functional abilities of people living with chronic pain. Patients who received mindfulness meditation training also had a reduction in symptoms of psychological distress such as depression and anxiety, and an overall reduction in pain medication use, which was not seen in patients who received standard care. Most patients maintained these benefits during a four-year follow-up.
- Lower blood glucose measurements in people with poorly controlled type 1 diabetes.
- Substantial improvement in pain levels, energy, sleep quality and overall well-being in a group of 77 patients undergoing treatment for fibromyalgia.
MSBR has also been shown to reduce recurrence rates in people treated for major depressive disorder, and to relieve depressive symptoms in people living with chronic illnesses such as HIV and diabetes, as well as organ transplant recipients.
Sources
“Center for Mindfulness”. UMass Memorial Health. https://www.ummhealth.org/services-treatments/center-mindfulness
“Mindfulness-Based Stress Reduction Research Summary”. University of Massachusetts Medical School. https://palousemindfulness.com/docs/research_summary.pdf
“Managing cancer pain with nonpharmacologic and complementary therapies”. Journal of the American Osteopathic Association. https://pubmed.ncbi.nlm.nih.gov/18165373/
“Everything You Need to Know About Fibromyalgia”. Healthline. https://www.healthline.com/health/fibromyalgia
“Mindfulness-based cognitive therapy as a treatment for chronic depression: A preliminary study”. Behavior Research and Therapy. https://pubmed.ncbi.nlm.nih.gov/19249017/
What Is Meditation?
July 8th, 2025Meditation and meditative practices embody a wide range of disciplines with dozens of different names. In general, however, these fall into four general categories:
- Contemplative meditation, in which the meditator focuses on an object, such as the breath, a sound (called a mantra), an image or a flame.
- Open awareness, in which the meditator seeks to open the mind to whatever is happening without focusing on any one thing. The Zen sitting practice of “zazen” is an example of this type of meditation.
- Mindfulness meditation is similar to contemplative meditation, but with a less narrow focus and an emphasis on noticing without judgment the distractions of the mind.
- Guided meditation, during which the meditator follows the voice of an instructor who guides them through a series of images, affirmations, feeling states (happiness, peacefulness) or experiences.
Studies show that all forms of meditation have a profound impact on the brain and measurable effects on thinking, behavior, learning and mood. These include the following:
- Preservation of brain mass: A study published in Frontiers in Psychology showed that long-term meditators had less gray-matter loss than non-meditators as they aged. (Gray matter is the part of the brain responsible for processing information — the human equivalent of a computer’s CPU.)
- Decreased “mind-wandering”: A 2011 study from Yale showed that meditating decreased activity in the brain’s “default mode network,” or DMN. This is the part of the brain that’s active when we are not thinking about anything in particular, the so-called “monkey brain.” When the DMN is active, we are more prone to ruminating and worrying about past or future events, which makes us more unhappy and more stressed.
- An antidepressant effect: According to a large meta-analysis by researchers at Johns Hopkins University, meditation had a small effect on symptoms associated with depression and anxiety. However, that effect was identical to that achieved with the use of antidepressant drugs.
- Improved attention and concentration: In a study done in 2013, researchers learned that only two weeks of meditation practice improved students’ performance on the graduate school entrance exam (GRE) by about 16 points.
- Change in size of key brain structures: A study from Harvard in 2011 showed that meditation increased the thickness of the hippocampus, a structure in the brain that governs learning and memory. Additionally, meditators had decreases in the volume of the amygdala, the part of the brain responsible for fear, anxiety and stress. What’s more, these physical changes were linked to self-reported improvements in feelings of well-being and mood.
- Help with addiction: According to several studies, just two weeks of meditation training can improve the success rate of smoking cessation efforts. In one study, meditation was better than the American Lung Association’s Freedom from Smoking Program in helping smokers to quit. There is also some evidence that mindfulness-based relapse prevention is better than conventional treatment in preventing relapse in people treated for substance abuse.
Additionally, research conducted by Michael Posner of the University of Oregon and Yi-Yuan Tang of Texas Tech University showed that meditators had changes in their brain’s white matter, the nerve fibers that allow brain regions to communicate with one another. Specifically, meditators had increased levels of myelin, the brain’s natural “insulation,” after only a few weeks of regular meditation practice. Posner believes that increased insulation helps different brain regions communicate faster and more efficiently.
Sources
“Forever Young(er): potential age-defying effects of long-term meditation on gray matter atrophy”. Frontiers in Psychology. https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2014.01551/full
“Meditation experience is associated with differences in default mode network activity and connectivity”. PNAS. https://www.pnas.org/doi/abs/10.1073/pnas.1112029108
“Meditation Programs for Psychological Stress and Well-being: A Systematic Review and Meta-analysis”. JAMA Internal Medicine. https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/1809754
“Mindfulness practice leads to increases in regional brain gray matter density”. PubMed Central. https://pmc.ncbi.nlm.nih.gov/articles/PMC3004979/
“Mechanisms of white matter change induced by meditation training”. Frontiers in Psychology. https://pmc.ncbi.nlm.nih.gov/articles/PMC4209813/
What Is Yoga?
July 8th, 2025Yoga is an ancient discipline that originated in India about 2,000 years ago. Although most Westerners think of it as a form of physical and mental exercise involving postures and breathing techniques, it was originally conceived as an ascetic practice and a path to enlightenment.
According to Chopra.com, the Indian sage Patanjali collated the 195 philosophical tenets behind the practice of yoga in the Yoga Sutras sometime between the 2nd and 4th centuries CE. This ancient Sanskrit text outlines the eight “limbs” of yoga:
- Yamas — correct behavior towards others: truthfulness, generosity and nonviolence
- Niyamas — guiding principles to live by: purity, contentment, study and devotion
- Asanas — body postures
- Pranayamas — breathing techniques
- Pratyahara — turning inward to explore the true self
- Dharana — training the mind to focus
- Dhyani — effortless meditation
- Samadhi — unity with the divine
According to the Sutras, the regular practice of these disciplines allows the mind to “settle into silence” and reveal one’s essential nature, which is unbounded consciousness.
Modern-day yoga, on the other hand, is a more physical practice, based heavily on asanas (postures) and breathing techniques. Created by Tirumalai Krishnamacharya in collaboration with gymnast and bodybuilding enthusiast Maharaja Krishnaraja Wodeyar IV, today’s yoga is actually a combination of traditional asanas, gymnastics and calisthenics with a smattering of meditative practice added in. Its primary goal is no longer the expansion of consciousness, but rather the maintenance of health and well-being. It is also considered a form of therapy.
Yoga’s health benefits
Like most Integrative health approaches, yoga has not yet been studied extensively by Western researchers. However, it does appear to have certain health benefits that can’t be attributed to exercise alone. For example, recent studies show that chronic low back pain responds well to certain “carefully adapted” yoga poses, says the National Center for Complementary and Integrative Health. Other studies suggest that yoga may help decrease the effects of stress on the body, including lowering blood pressure and heart rate. There is also some evidence that yoga may help prevent or relieve tension headaches, alleviate symptoms of anxiety and depression, and improve sleep.
Yoga and yoga therapy have also been shown to be a beneficial adjunct in palliative care. Although people with advanced disease may be too ill to participate, many yoga poses can be adapted for people who are chronically ill, and may be especially helpful when combined with mindfulness meditation and breathing techniques. Some observed benefits in women with advanced breast cancer who were taught to do yoga at home included a lessening of disease impact and an improved sense of well-being. Gentle yoga combined with breathing exercises and mindfulness have also been shown to help patients manage cancer-related pain and fatigue.
With that being said, yoga can be physically taxing, and may lead to injuries if not properly performed. According to the NCCIH, the most common injuries are sprains and strains, especially of the lower legs and knees. You can reduce your risk of injury by working with a trained instructor who can help you adapt your practice to match your skill level and physical abilities. And, as with all forms of exercise, you should check with your health care provider before you enroll in a yoga class. This is particularly important if you have health conditions such as glaucoma, high blood pressure or sciatica, or if you are pregnant.
Sources
“Mindfully Mortal”. https://www.kenbreniman.com/
“Yoga: Effectiveness and Safety”. National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/yoga-effectiveness-and-safety
“Yoga for palliative care”. Integrative Medicine Research. https://pmc.ncbi.nlm.nih.gov/articles/PMC6160500/
What Is Spinal Manipulation?
July 8th, 2025Spinal manipulation refers to a wide array of techniques that are used to treat a number of medical conditions, most commonly back and neck pain. According to Spine-Health, the usual goal of spinal manipulation is to “restore or enhance joint function, with the general goals of resolving joint inflammation and reducing pain.” However, most practitioners of spinal manipulation believe that improper spinal alignment has a profound effect on the body as a whole, and that correcting misalignment in the spine can improve overall health.
Spinal manipulation may be performed by either a chiropractor or an osteopathic physician. Both professions employ a variety of techniques, but chiropractors typically focus on spinal adjustments, whereas an osteopathic physician may employ many different modalities, including massage, pressure and mobilization of other joints. Additionally, an osteopathic physician is a medical doctor who can diagnose illnesses, perform surgery and prescribe medications. Chiropractors are not medical doctors, although they receive an extensive postgraduate education and must pass an exam to be licensed by the state. (Note: Many European countries and Canada offer osteopathic training, but these professionals are not medical doctors and cannot practice medicine in the U.S.)
There are over 100 different techniques used in spinal manipulation, which generally fall into two broad categories: high-velocity, low-amplitude thrust, or low-force, gentle techniques. The former is the one with which most people are familiar, and involves positioning the patient in a certain way and then moving a joint suddenly, typically creating an audible “pop.” The second group of techniques involves less forceful movements. Often called spinal mobilization, these techniques are preferred by some practitioners, especially for patients who are small or frail or have certain medical conditions such as osteoporosis or nervous system disorders.
Efficacy of Spinal Manipulation
Research supports the use of spinal manipulation techniques for a number of conditions. According to WebMD, it is often effective for neck pain, headaches, osteoarthritis and fibromyalgia, and may be of some benefit for low back pain. However, it’s important to note that people with certain medical conditions, such as osteoporosis, inflammatory arthritis, spinal cord compression or some forms of cancer should avoid spinal manipulation, as it may cause harm. People who are taking blood thinners such as warfarin or Xarelto or those with known degenerative disc disease, should be cautious as well. Although rare, spinal manipulation has been known to worsen herniated discs or cause spinal cord compression in patients with underlying disc disease or a history of trauma to the back or spine.
Sources
“What is a Chiropractor?”. Spine-Health. https://www.spine-health.com/treatment/chiropractic/what-a-chiropractor
“What Training Do Chiropractors Have and What Do They Treat?” Healthline. https://www.healthline.com/health/are-chiropractors-doctors
“Chiropractic Adjustment for Back Pain”. WebMD. https://www.webmd.com/back-pain/chiropractic-pain-relief#1
“Fibromyalgia”. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/fibromyalgia/symptoms-causes/syc-20354780
“What Is Degenerative Disc Disease?”. Spine-Health. https://www.spine-health.com/conditions/degenerative-disc-disease/what-degenerative-disc-disease
What Is Acupuncture?
July 8th, 2025Acupuncture is a technique used in traditional Chinese medicine that acts to redirect the flow of the body’s vital energy, known as “qi” (pronounced “chee”). In traditional acupuncture, a trained practitioner inserts very thin needles about the size of a human hair into designated points along a “meridian” (a path in the body along which qi flows). According to John Pirog, MSOM, of Northwestern Health Sciences University, there are 12 meridians in all, each of which corresponds to a particular organ in the body. “Yin” meridians typically correspond to organs without an empty cavity, such as the heart, liver, spleen and kidney. “Yang” meridians correspond to organs that have an empty cavity, such as the stomach, gallbladder and intestines. By stimulating points along a particular meridian, the acupuncture practitioner balances the flow of energy and provokes therapeutic change in the corresponding organ, Pirog explains.
Although acupuncture employs needles, when done properly, the procedure rarely hurts. Most patients report no sensation at all or a mild feeling of pressure when the needles are inserted. With that being said, some acupuncture points may be more sensitive than others, especially those on the hands and feet. Additionally, some practitioners stimulate acupuncture points further by heating the needles with a mild electrical current, which creates a “pins and needles” effect. In any case, discomfort should be very mild and brief. If it isn’t, you should let your practitioner know.
In addition to needles, an acupuncturist may use other forms of stimulation to redirect the flow of qi. These include the following:
- Vacuum pressure (“cupping”)
- Application of heat (“moxibustion”)
- Mild electrical current (electroacupuncture)
- Chinese massage (tui na)
- Chinese exercise system (tai ji)
Does acupuncture work?
Practitioners of traditional Chinese medicine have used acupuncture to successfully treat various ailments for about 2,500 years. Here in the West, it first gained popularity as a Integrative therapy in the 1990s, when the FDA approved acupuncture needles as a medical device. In the two decades since that time, multiple studies have confirmed that acupuncture does, in fact, work, says Hopkins Medicine. The conditions that have been successfully treated with either acupuncture alone or acupuncture in combination with more traditional Western therapies include the following:
- Asthma
- Post-surgical dental pain
- Headaches
- Fibromyalgia
- Addiction
- Tennis elbow
- Low back pain
- Osteoarthritis
- Menstrual pain
Additionally, a 2012 study in which researchers conducted an analysis of four large randomized controlled studies on the efficacy of acupuncture for chronic pain found acupuncture to be superior to both no treatment and “sham” acupuncture for four chronic pain conditions: chronic migraines, neck and back pain, osteoarthritis and shoulder pain.
Sources
“What is the Meridian System?” Shen Nong. http://www.shen-nong.com/eng/principles/whatmeridian.html
“What is acupuncture?”. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/wellness-and-prevention/acupuncture
“Acupuncture for Chronic Pain”. JAMA Internal Medicine. https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/1357513
